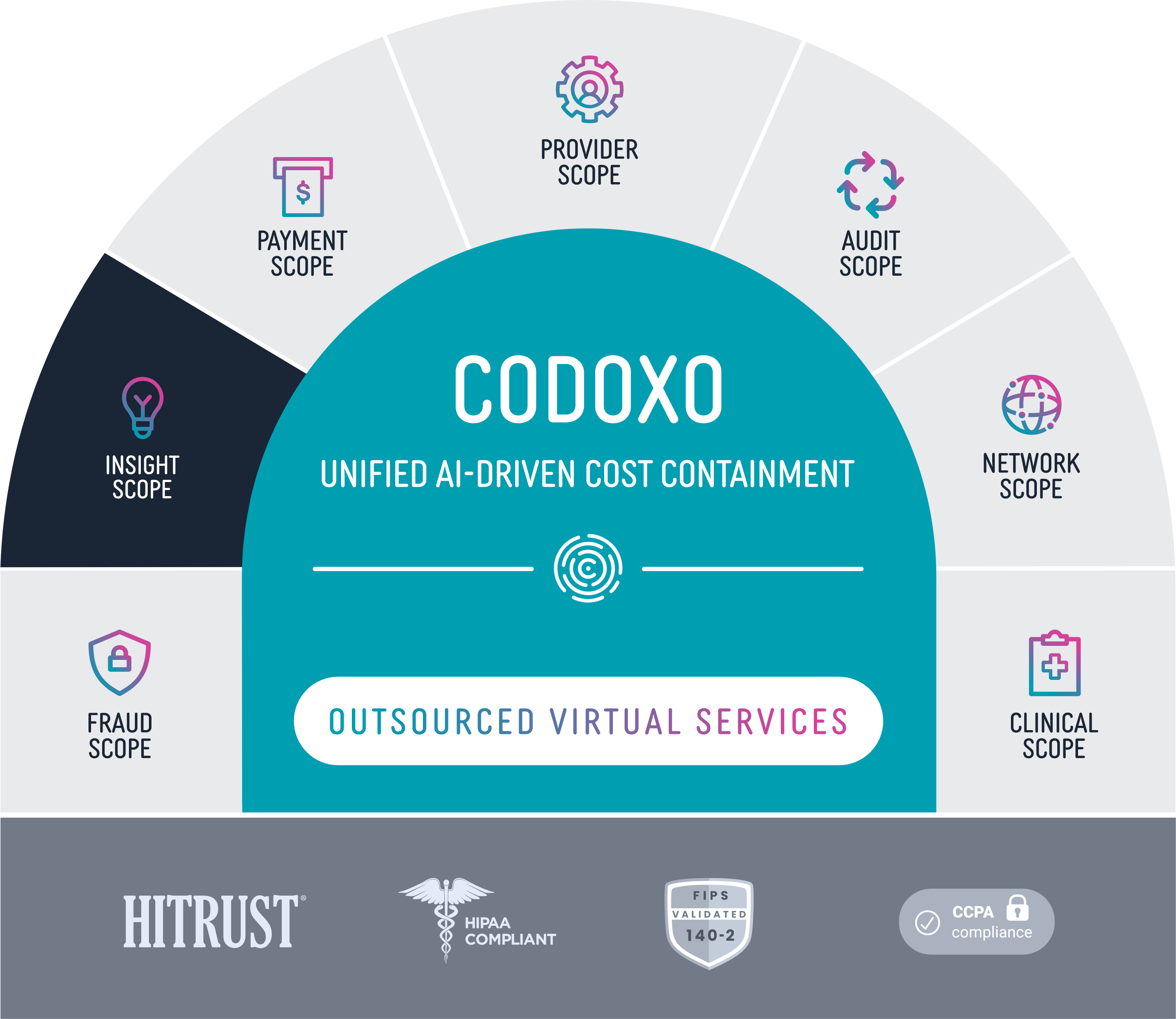
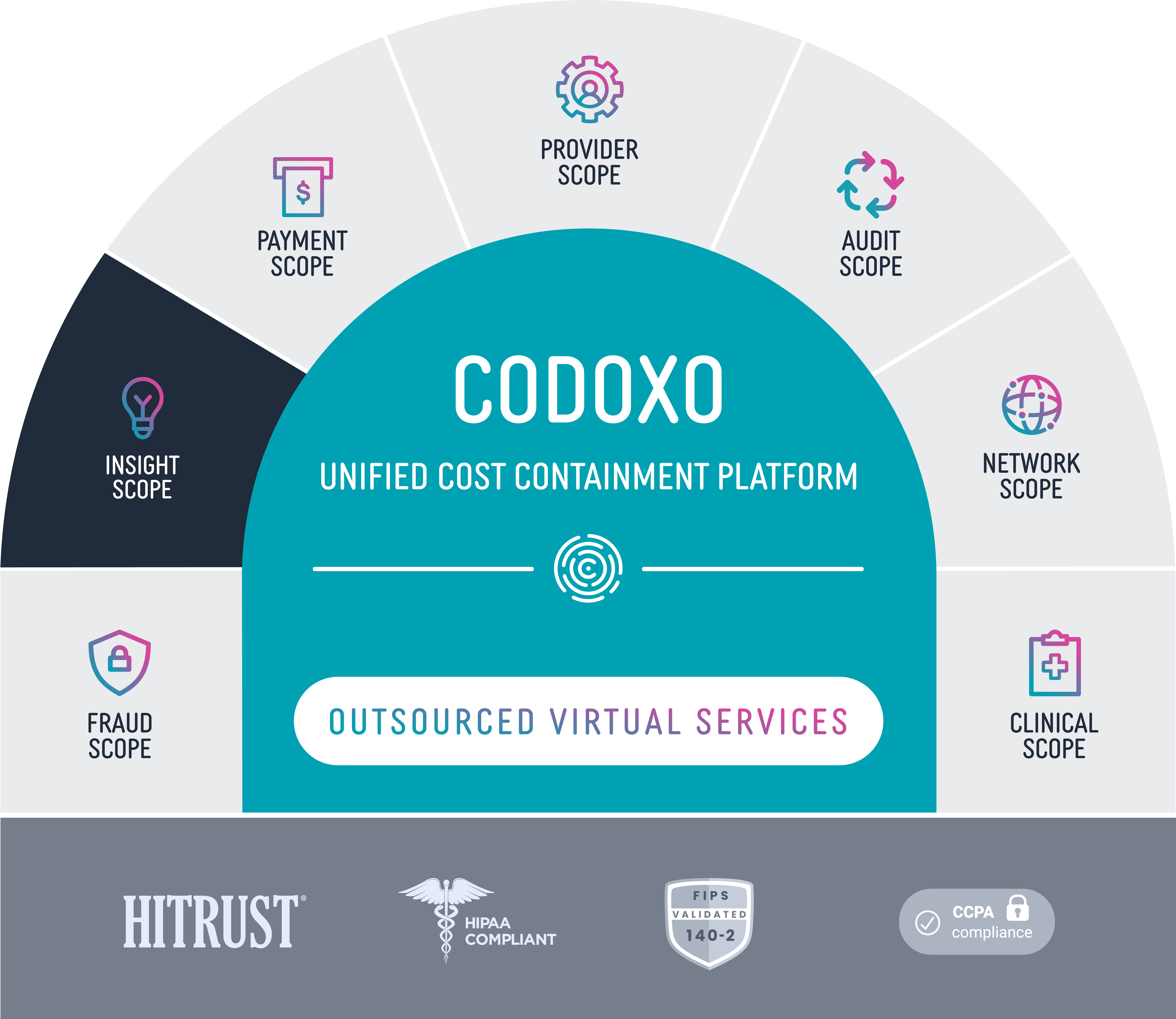
Insight Scope
Democratize access to claim, provider, facility and member insights and behavior-based context with easy-to-use reports and queries
Insight Scope gives everyone across your healthcare company or agency an easy way to research issues with self-service reporting and querying of claim, provider, facility and member behavior. Easy-to-use queries and reports make it easy for anyone to take the initiative, follow the data, and act quickly to address problems.
Our healthcare insurance AI software is popular with Clinical Care, Medical Management, Claims Operations and Health Strategy teams because of everything it lets you do:
Easy-to-use queries
to search for any claim, claim line, provider, facility, pharmacy, behavioral, dental or workers comp record. Results can also be aggregated by rendering or billing entity.
Self-service reports
to access relevant data, filter, sort, visualize and analyze claims, provider, facility, and member behavior over time – without any help from IT.
Unique behavior insights
into problematic insurance claims and provider activity.
Location analysis
makes it easy to see where claims and providers are in relation to each other with a familiar ‘map view’.
Association graphs
based on user preference and filtering criteria to map connections between providers or entities.
Code utilization
views that allow users to identify codes that have frequency and cost for various providers and entities.
AI-based claims risk score
flags suspicious activity accurately and with low false positives. Detailed explanations of each claims risk score are available with the Fraud Scope or Payment Scope application.
Provider integrity score
flags providers associated with suspicious claims activity or with coding practices that fall outside the norm of their peers. Detailed explanations for the provider integrity score are available with the Fraud Scope application.
Scheme dashboard
gives everyone a high-level look at the various schemes that exist in your insurance plan. Detailed scheme explanations are available with the Fraud Scope application.
Watch lists
for problematic providers and facilities that may be involved in FWA activity as determined by the Codoxo Forensic AI platform and your existing teams.
Whitelist
providers and facilities that you do not want to analyze.
Collaborative workflows
make it easy to share data and reports with others across your organization, accelerating research and resolution for everything from network and clinical questions to payment integrity and fraud issues.
Enrich insights with additional data
you have about each provider, network and plan.
Augment analysis with third party data
such as OIG or state exclusion lists.
AI analyzes
all claim types
Codoxo can ingest and analyze all professional, facility, pharmaceutical, behavioral, dental, and workers comp claims.
AI analyzes
all CODES
Our patented AI technology has the ability to identify issues and opportunities that may arise from complex claims and codes in addition to the standard ones which helps discover a wider range of existing and emerging problems.
Insight Scope is built on our Forensic AI Platform and a part of the Codoxo Unified Cost Containment Platform
Our AI engine analyzes your claims data, detects providers and entities that intentionally or unintentionally waste money, and builds connections across your data to provide actionable insights.

We invest heavily in our people and our technology to help us push the boundaries of what’s possible.
We have helped achieve savings at world-class payers and healthcare agencies including:
Highmark
6+ million members
State Medicaid Agency
1.5+ million recipients
Southeast Health Plan
3.5+ million members
Pacific Health Plan
700k+ members
Mid-State Health Plan
3.5+ million members
Midwest Plan
2.5+ million members

We invest heavily in our people and our technology to help us push the boundaries of what’s possible.
We have helped achieve savings at world-class payers and healthcare agencies including:
Highmark
6+ million members
State Medicaid Agency
1.5+ million recipients
Southeast Health Plan
3.5+ million members
Pacific Health Plan
700k+ members
Mid-State Health Plan
3.5+ million members
Midwest Plan
2.5+ million members
Ready for a better solution?
Request a demo to learn what we can do for you.