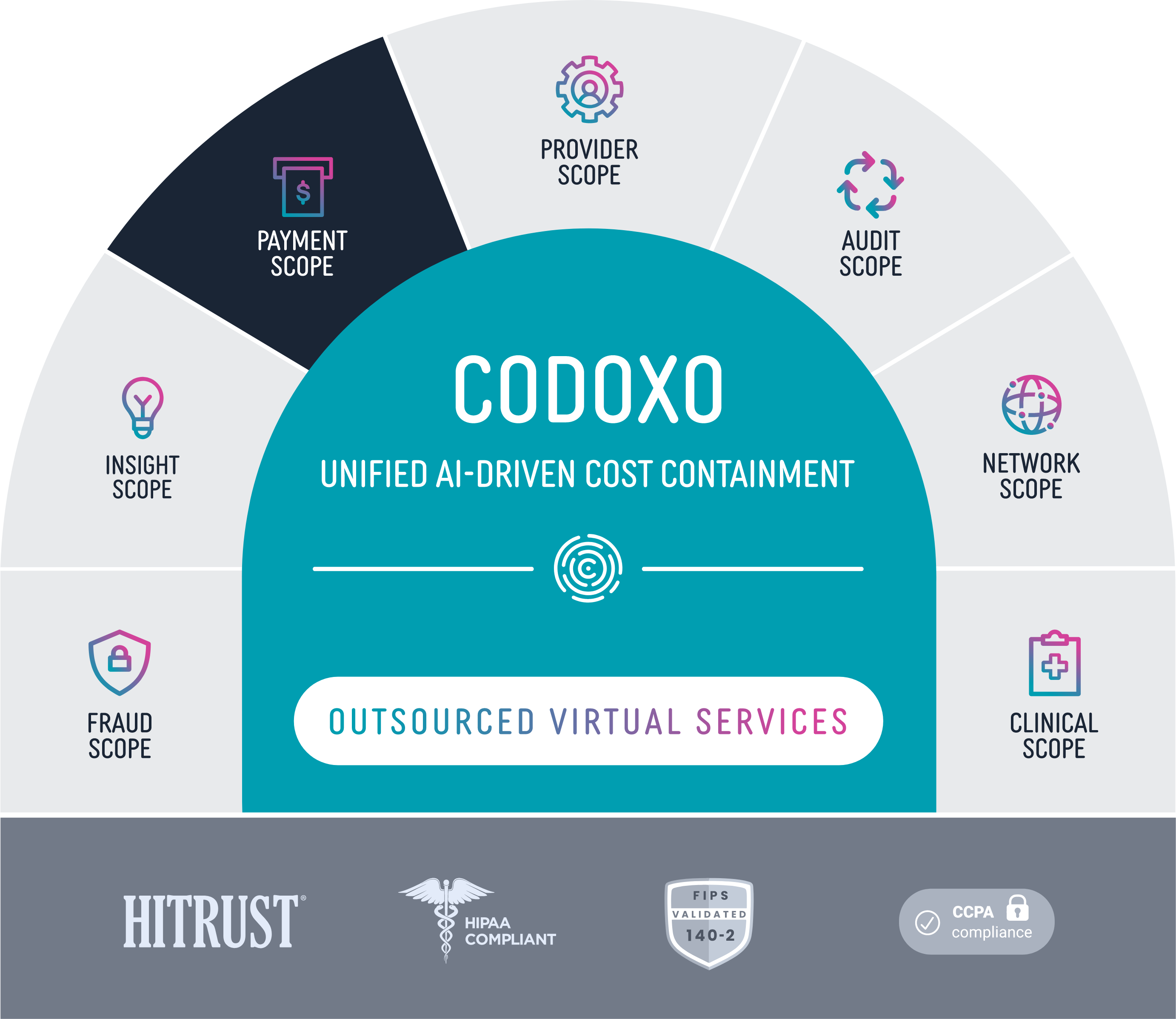
Payment Scope
Identify claim accuracy issues before claims are paid with our patented Forensic AI engine for payment integrity
Payment Scope proactively flags problematic claims and helps analysts save costs pre-payment with unique claim insights, easy-to-use claim workflow, and automated provider outreach.
AI analyzes claims pre-payment
and assigns risk scores to claims along with detailed explanations that help identify problematic claims.
Gives analysts integrated workflows
to approve, deny or pend each claim with a reason code.
Significantly lower provider abrasion
with integrated approach to AI problem identification.
Customize results
using watchlists, whitelists, and claim amount thresholds.
Provider Integrity Score
flags providers associated with any new or existing fraud schemes, or with coding practices that fall outside the norm of their peers. Detailed explanations for the provider integrity score are available with the Fraud Scope application.
Claims dashboard
gives all users an at-a-glance overview of the current claims review workflow as well as a breakdown of claims by risk scores and potential savings.
Analyst dashboard and workflow screens
give each user an easy way to review each claim, understand the reason why a claim was flagged, request more information from a provider, update claim notes, and move the claim through your review workflow.
Automate claims reviews
with real-time integration to your claims system and automatically pend or deny payments for high-risk claims with suspicious activity.
Ensure contract payment accuracy
with integrated pre-pay and contract analysis.
AI analyzes
all claim types
Codoxo can ingest and analyze all professional, facility, pharmaceutical, behavioral, dental, and workers comp claims.
AI analyzes
all CODES
Our patented AI technology has the ability to identify issues and opportunities that may arise from complex claims and codes in addition to the standard ones which helps discover a wider range of existing and emerging problems.
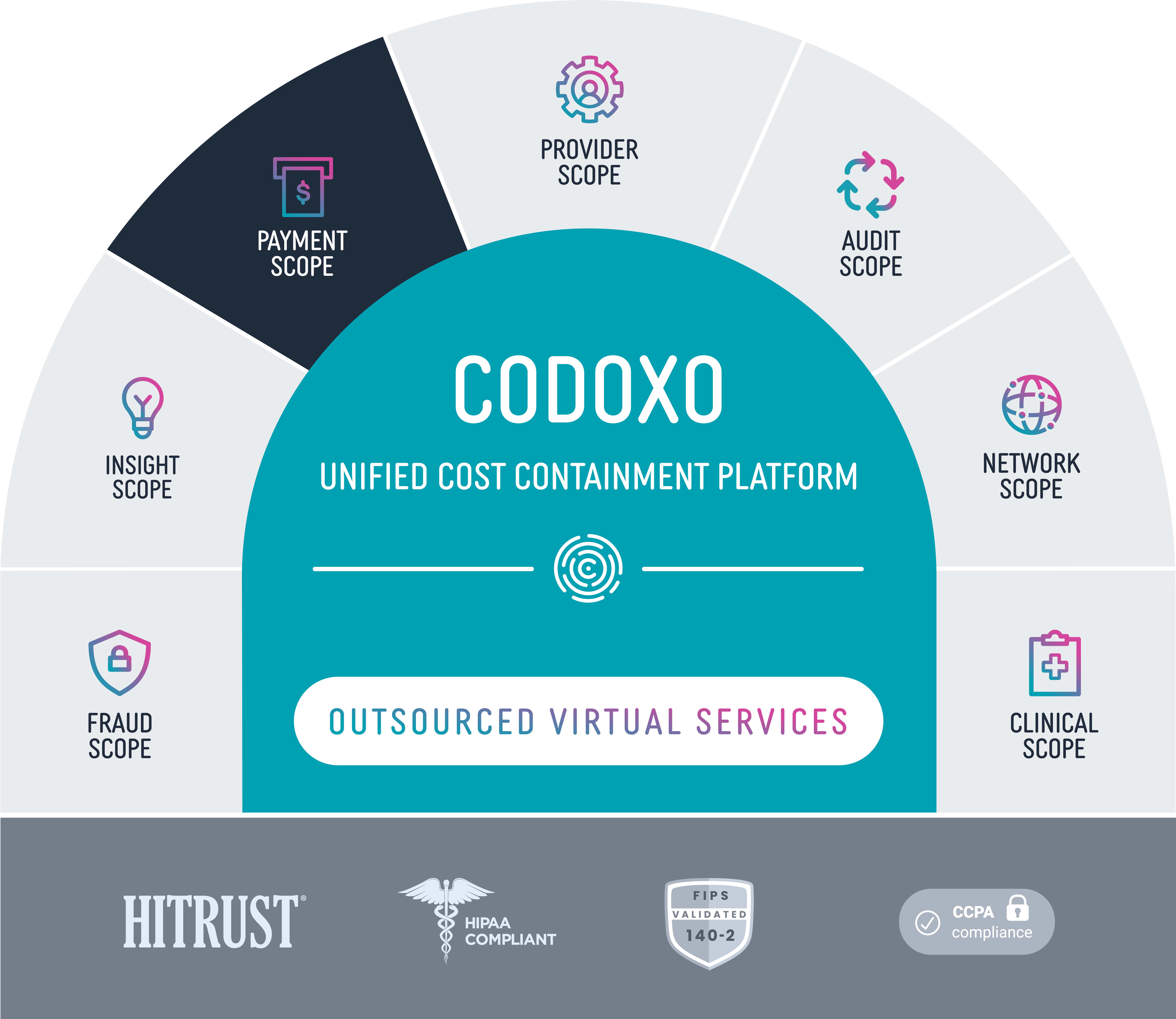
Payment Scope is built on our Forensic AI Platform and a part of the Codoxo Unified Cost Containment Platform
Our AI engine analyzes your claims data, detects practices that intentionally or unintentionally waste money, and builds connections across your data to provide actionable insights.

We invest heavily in our people and our technology to help us push the boundaries of what’s possible.
We have helped achieve savings at world-class payers and healthcare agencies including:
Highmark
6+ million members
State Medicaid Agency
1.5+ million recipients
Southeast Health Plan
3.5+ million members
Pacific Health Plan
700k+ members
Mid-State Health Plan
3.5+ million members
Midwest Plan
2.5+ million members

We invest heavily in our people and our technology to help us push the boundaries of what’s possible.
We have helped achieve savings at world-class payers and healthcare agencies including:
Highmark
6+ million members
State Medicaid Agency
1.5+ million recipients
Southeast Health Plan
3.5+ million members
Pacific Health Plan
700k+ members
Mid-State Health Plan
3.5+ million members
Midwest Plan
2.5+ million members
Ready for a better solution?
Request a demo to learn what we can do for you.